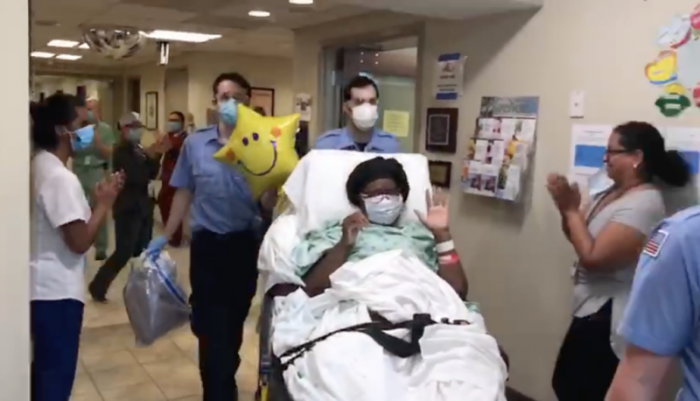
Connection and Communication: Powerful Forces on COVID Unit
Marian Steele, shown above with her husband Robert, remembers vividly the April day she was transferred to RML Specialty Hospital, recovering from COVID-19 and on a ventilator.
“I hadn’t seen my family in almost four weeks, I couldn’t talk, and now they were taking me by ambulance to someplace even further away,” she recalled. “I was so anxious. But when I got to the hospital, I was surrounded by people who told me they were going to take care of me. They changed my gown and washed me. They treated me like I was their mom, or their sister or their auntie. They put my mind at ease.”
Ms. Steele was one of the earliest patients treated on the dedicated COVID unit at RML Specialty Hospital in Hinsdale. By the time she arrived, she had already been on a ventilator for nearly three weeks and she desperately wanted to see her husband, Robert. Ms. Steele was about to discover two things: her team members were experts at helping patients learn to breathe on their own again and they were also now her new family – at least for the time being.
RML Steps Up When Acute Care Hospitals Call for Help
Clinical Outcomes Impressive
In the early months of 2020, COVID-19 evolved rapidly in the United States from a handful of isolated cases to a full-blown crisis, stressing the fabric of communities and every aspect of daily life. Hospitals were full, and COVID patients who needed ventilator support to breathe were stretching the capacity of intensive care units. As one of the nation’s leading ventilator-weaning hospitals, RML had a unique role to play.
In very short order, the hospital opened dedicated COVID units at both the Hinsdale and Chicago locations, developing extensive safety protocols to protect patients and staff. They then asked for volunteers. Despite possible risks to their own health and the health of their families, employees from both hospitals stepped up without hesitation. By mid-April, the units were admitting new patients every day.
The clinical results have been impressive. RML teams have been so effective that, to date, they have cared for 105 ventilator-dependent patients. Of these, 95 or 90%, have been successfully weaned from their ventilators and 65, or 62%, have been discharged either to their home or to an acute rehabilitation center. Two research studies about these results are expected to be published in the near future.
While the clinical successes of the COVID unit are significant, though, staff members say that something else happened in this unique environment as well. Patients and staff formed bonds that will last a lifetime.
Becoming a Family
Support, Encouragement and Communication Make the Difference

For Marian Steele, there were days when she couldn’t tell the difference between reality and hallucination, but the personal support she received gave her the will to keep trying.
For 24-year-old Olivia Vecchiet, the unit’s certified occupational therapy assistant (COTA), the experience was “transformational. I will never forget this time with my patients and with this team. I’m just two years into my career, but this experience will be with me forever.”
What made this situation so different from others? “I discovered just how important emotional support is – for everyone,” said Joy Magundayao, a respiratory therapist who has been with RML for 12 years. “We were all scared, but the hospital did everything possible to keep us safe and we felt supported by leadership and people in every department. We’d see people walk by the door to the unit and wave to us through the window for moral support. That was great.
“With our patients, we were the only ones at the bedside, day in and day out,” Ms. Magundayao continued. “I became closer to my patients than ever before. I knew the little things they needed, like a nail file or a nail clipper, and I made sure to bring those things in. We touched them, we held their hands. These things had a big impact – on them and on us.”
Staff members who worked on the unit said they recognized just how frightening the new COVID environment could be for everyone. “For family members, it was devastating to take a very sick loved one to the emergency department, be told they had to be put on a ventilator, and then be asked to leave because of the no-visitor policy,” said Amy Grissette, RN, BSN, the unit’s nurse manager. “And for our patients, in particular, they were waking up in a different hospital from where they started. It was unfamiliar, and they wanted their families.”

The team and the hospital did everything to keep people as connected as possible, Ms. Grissette said. “So that patients could see their loved ones, we conducted virtual visits with families by either using their personal cell phone or laptop, or by using iPads purchased by RML,” she explained. “Our nurses also called family members daily. Some families were having a very hard time, and our nurses became their counselors and support system.”
Although this level of responsibility could be draining at times, Ms. Grissette was also inspired by the dedication of the COVID team. “There was a lot of bonding on the unit,” she said. “We truly became a family, working together, with no person left behind. Our mission was to help our patients return back to their families.”
Jillian Childs, PT, DPT, a physical therapist, was impressed with the extensive communication the team was able to have “on a constant basis. Everyone was always on the unit, so we could bounce ideas off of everyone together, anytime we needed. It really helped us move our patients forward.”
First Moments of Awareness, First Steps toward Recovery
One of the team’s biggest challenges happened to be RML’s area of expertise: helping patients through the process of waking up in unfamiliar surroundings and learning to breathe again on their own, without the support of the ventilator.
“Most people have no idea how terrifying this is,” said Ms. Magundayao. “Patients often cry when they first wake up, and they can be quite agitated. They don’t know where they are. Because they’ve been so sick, they often imagine things and have hallucinations during this period.”
Marian Steele was one of those people. “I couldn’t tell what was real and what was a dream,” she recalled.
“I was convinced that I’d had a terrible verbal confrontation with a woman at my church. I really wanted to apologize. Turns out, it never happened, but I was absolutely sure that it had.”

Marian also had to be slowly weaned from the ventilator, and by the time she was breathing completely on her own, she had been using ventilator support for nearly six weeks. “This is what we do every day for patients across our hospital, but we learned that with our COVID patients, we had to go more slowly,” said Ms. Magundayao. “When the ventilator has been doing the work of breathing for you for so long, you really have to give the lungs and the body time to adjust.”
For Marian, staff encouragement helped her turn the corner, and the long-anticipated family ‘visit’ worked like magic.
“I had just been trying to stand for the first time, and I was so broken-hearted when I couldn’t do it,” she recalled. “It felt like I was weighed down with cinder blocks. The day arrived when my whole family was coming to see me through my hospital window, but I wasn’t sure I would be able to stand up. Olivia was with me, though, and she shouted out to them, ‘She’s going to stand, she’s going to stand.’ And then I just had to do it. She helped me to the window, and the family was applauding, screaming and crying. They had made ‘Woman of Steele’ posters because that’s my nickname. It was an amazing feeling.”
Olivia Vecchiet, the certified occupational therapy assistant, had actually started working on the unit as a patient care technician (PCT) because the hospital wasn’t yet assigning physical or occupational therapists. As a PCT, she provided intimate and supportive care for Ms. Steele, and they became close. She remembers vividly the Steele family visit. “It was so emotional, so happy. All of my fears of COVID left me for a moment and it felt wonderful.”
A Final Plea for Safety
After more than two months in three different hospitals, Ms. Steele was thrilled to return home to her husband, Robert, in early June. Mr. Steele didn’t “deal well” with being separated from his wife of 30 years. “She is my sweetheart. It was really hard when she was so sick.” He has a message for the world: “Whatever you’re told to do to keep people from getting sick, please do it. Wear a mask, stay home if you can. Stay far apart. It’s important. This is serious.”


 For Marian Steele, there were days when she couldn’t tell the difference between reality and hallucination, but the personal support she received gave her the will to keep trying.
For 24-year-old Olivia Vecchiet, the unit’s certified occupational therapy assistant (COTA), the experience was “transformational. I will never forget this time with my patients and with this team. I’m just two years into my career, but this experience will be with me forever.”
What made this situation so different from others? “I discovered just how important emotional support is – for everyone,” said Joy Magundayao, a respiratory therapist who has been with RML for 12 years. “We were all scared, but the hospital did everything possible to keep us safe and we felt supported by leadership and people in every department. We’d see people walk by the door to the unit and wave to us through the window for moral support. That was great.
“With our patients, we were the only ones at the bedside, day in and day out,” Ms. Magundayao continued. “I became closer to my patients than ever before. I knew the little things they needed, like a nail file or a nail clipper, and I made sure to bring those things in. We touched them, we held their hands. These things had a big impact – on them and on us.”
Staff members who worked on the unit said they recognized just how frightening the new COVID environment could be for everyone. “For family members, it was devastating to take a very sick loved one to the emergency department, be told they had to be put on a ventilator, and then be asked to leave because of the no-visitor policy,” said Amy Grissette, RN, BSN, the unit’s nurse manager. “And for our patients, in particular, they were waking up in a different hospital from where they started. It was unfamiliar, and they wanted their families.”
For Marian Steele, there were days when she couldn’t tell the difference between reality and hallucination, but the personal support she received gave her the will to keep trying.
For 24-year-old Olivia Vecchiet, the unit’s certified occupational therapy assistant (COTA), the experience was “transformational. I will never forget this time with my patients and with this team. I’m just two years into my career, but this experience will be with me forever.”
What made this situation so different from others? “I discovered just how important emotional support is – for everyone,” said Joy Magundayao, a respiratory therapist who has been with RML for 12 years. “We were all scared, but the hospital did everything possible to keep us safe and we felt supported by leadership and people in every department. We’d see people walk by the door to the unit and wave to us through the window for moral support. That was great.
“With our patients, we were the only ones at the bedside, day in and day out,” Ms. Magundayao continued. “I became closer to my patients than ever before. I knew the little things they needed, like a nail file or a nail clipper, and I made sure to bring those things in. We touched them, we held their hands. These things had a big impact – on them and on us.”
Staff members who worked on the unit said they recognized just how frightening the new COVID environment could be for everyone. “For family members, it was devastating to take a very sick loved one to the emergency department, be told they had to be put on a ventilator, and then be asked to leave because of the no-visitor policy,” said Amy Grissette, RN, BSN, the unit’s nurse manager. “And for our patients, in particular, they were waking up in a different hospital from where they started. It was unfamiliar, and they wanted their families.”
 The team and the hospital did everything to keep people as connected as possible, Ms. Grissette said. “So that patients could see their loved ones, we conducted virtual visits with families by either using their personal cell phone or laptop, or by using iPads purchased by RML,” she explained. “Our nurses also called family members daily. Some families were having a very hard time, and our nurses became their counselors and support system.”
Although this level of responsibility could be draining at times, Ms. Grissette was also inspired by the dedication of the COVID team. “There was a lot of bonding on the unit,” she said. “We truly became a family, working together, with no person left behind. Our mission was to help our patients return back to their families.”
Jillian Childs, PT, DPT, a physical therapist, was impressed with the extensive communication the team was able to have “on a constant basis. Everyone was always on the unit, so we could bounce ideas off of everyone together, anytime we needed. It really helped us move our patients forward.”
The team and the hospital did everything to keep people as connected as possible, Ms. Grissette said. “So that patients could see their loved ones, we conducted virtual visits with families by either using their personal cell phone or laptop, or by using iPads purchased by RML,” she explained. “Our nurses also called family members daily. Some families were having a very hard time, and our nurses became their counselors and support system.”
Although this level of responsibility could be draining at times, Ms. Grissette was also inspired by the dedication of the COVID team. “There was a lot of bonding on the unit,” she said. “We truly became a family, working together, with no person left behind. Our mission was to help our patients return back to their families.”
Jillian Childs, PT, DPT, a physical therapist, was impressed with the extensive communication the team was able to have “on a constant basis. Everyone was always on the unit, so we could bounce ideas off of everyone together, anytime we needed. It really helped us move our patients forward.”
 Marian also had to be slowly weaned from the ventilator, and by the time she was breathing completely on her own, she had been using ventilator support for nearly six weeks. “This is what we do every day for patients across our hospital, but we learned that with our COVID patients, we had to go more slowly,” said Ms. Magundayao. “When the ventilator has been doing the work of breathing for you for so long, you really have to give the lungs and the body time to adjust.”
For Marian, staff encouragement helped her turn the corner, and the long-anticipated family ‘visit’ worked like magic.
“I had just been trying to stand for the first time, and I was so broken-hearted when I couldn’t do it,” she recalled. “It felt like I was weighed down with cinder blocks. The day arrived when my whole family was coming to see me through my hospital window, but I wasn’t sure I would be able to stand up. Olivia was with me, though, and she shouted out to them, ‘She’s going to stand, she’s going to stand.’ And then I just had to do it. She helped me to the window, and the family was applauding, screaming and crying. They had made ‘Woman of Steele’ posters because that’s my nickname. It was an amazing feeling.”
Olivia Vecchiet, the certified occupational therapy assistant, had actually started working on the unit as a patient care technician (PCT) because the hospital wasn’t yet assigning physical or occupational therapists. As a PCT, she provided intimate and supportive care for Ms. Steele, and they became close. She remembers vividly the Steele family visit. “It was so emotional, so happy. All of my fears of COVID left me for a moment and it felt wonderful.”
Marian also had to be slowly weaned from the ventilator, and by the time she was breathing completely on her own, she had been using ventilator support for nearly six weeks. “This is what we do every day for patients across our hospital, but we learned that with our COVID patients, we had to go more slowly,” said Ms. Magundayao. “When the ventilator has been doing the work of breathing for you for so long, you really have to give the lungs and the body time to adjust.”
For Marian, staff encouragement helped her turn the corner, and the long-anticipated family ‘visit’ worked like magic.
“I had just been trying to stand for the first time, and I was so broken-hearted when I couldn’t do it,” she recalled. “It felt like I was weighed down with cinder blocks. The day arrived when my whole family was coming to see me through my hospital window, but I wasn’t sure I would be able to stand up. Olivia was with me, though, and she shouted out to them, ‘She’s going to stand, she’s going to stand.’ And then I just had to do it. She helped me to the window, and the family was applauding, screaming and crying. They had made ‘Woman of Steele’ posters because that’s my nickname. It was an amazing feeling.”
Olivia Vecchiet, the certified occupational therapy assistant, had actually started working on the unit as a patient care technician (PCT) because the hospital wasn’t yet assigning physical or occupational therapists. As a PCT, she provided intimate and supportive care for Ms. Steele, and they became close. She remembers vividly the Steele family visit. “It was so emotional, so happy. All of my fears of COVID left me for a moment and it felt wonderful.”